The manuscript of this recent musing about perhaps the most important component of my career in rheumatology was just accepted for publication in Clinical Medicine, after being rejected by a surgical journal. Sometimes those blades just can’t take a joke. For you outsiders: blades are surgeons, for obvious reasons, whereas we internists, with our focus on poking patients and drawing all that blood, are the fleas.
Who let this flea in my operating room?
Robert W. Ike
Abstract
Adoption by one specialty of a technique strongly identified with another never proceeds smoothly. A decision in the early 1980s by one of the movers and shakers of American Internal Medicine that rheumatologists should adopt arthroscopy involved this author as the spearhead of that effort. What follows is a recollection of how that went.
That happened at my University of Michigan back in ’87. My chief of medicine, Bill Kelley, was fond of pushing borders to insert internists into niches where they weren’t necessarily welcome, all in the interest of expanding internal medicine into developing areas where they might make a contribution. A rheumatologist, Kelley became president of the American Rheumatism Association (ARA, now American College of Rheumatology) in ’85 and in his ’86 presidential address to the annual meeting, took on the problem we were seeing of flagging interest in our subspecialty by medical students and trainees. Among the remedies he stated was “I believe we need to expand the specialty of rheumatology to cover some of the peripheral areas which now are largely ignored and sometimes poorly handled. This would include …the use of certain technical procedures which are appropriate to our specialty” (my emphasis) (1). At the time, I already had my new job, and the charge that came with it, but it was nice to hear marching orders. I was having a pretty good time as a rheumatology fellow when the call came. The clinical side was a blast, and the lab was where you put in your dues to get a good clinical job. It was my lab mentor who told me they were looking for someone to learn arthroscopy, and I was their top candidate. I thought I’d caught Kelley’s eye with my recent presentation of a patient I’d diagnosed with Brucellosis. Kelley’s protegée, my attending, friend, later best man, and eventual division chief Tommy Palella, had clued him in to the case so he showed up. So Kelley knew I was a sharp dude. Only several years later did I learn what about me actually caught his eye. His son, Mark, an eventual gastroenterologist, was an intern on my service. Mark confided to me that what his dad really liked was my size (I’m 6’8” tall), as one thing orthopods respect is size. Since my height probably got me into medical school (Dean Ceithaml of U of Chicago, who loved jocks, mistook my response about playing basketball at Michigan “I.M.” (for intramurals) as “I am”), what’s one more opened door? Just hope I don’t hit my head on the transom.
That meant a year away from my just purchased house and soon to be married bride as I moved into Lincoln Park to be near Augustana Hospital (reportedly favored by the area mafiosi) to be near where Bill Arnold did his arthroscopies. Bill had been Kelley’s first fellow at Duke, a handsome, charismatic, incredibly bright guy who was going places. He landed back at University of Illinois, where he (and Tommy Palella) had gone to med school. Bill’s lab work on purines was well received, but he chafed at the institution and struck out on his own, looking for new things. A few rheumatologists had been dabbling in arthroscopy in the 70s, but improvements in the procedure were making it more accessible. After talking with some orthopedic bigwigs about getting involved, and being encouraged, he was directed to Dave Stuhlberg at Northwestern, who was interested in all types of surgery for arthritis and with Bill set up a combined rheumatology -orthopedics arthroscopy unit at a small community hospital. There, Bill cut his chops sufficiently to go independent. I don’t know which Bill floated the idea of training someone, but there I was, welcomed with open arms. It had to be a big validation to Bill’s venture that a major academic rheumatology unit was investing a charge in his hands. It was all new to me. I’d hated my surgery rotations in med school – the early rise to hang around in pajamas doing nothing, the washing rituals, all the standing around – but scrubs and scrubbing were part of this deal. There was no standing around with Bill in the O.R. From the start my hands were on the equipment. Since scopes were videotaped, the post-game review was part of the process, although it could be accomplished in my Stressless recliner before the TV holding a suitable beverage.
Re-entry to the U required many a beverage. Bill Kelley was the most powerful man in the medical center, but imposing his will on the Department of Surgery proved more difficult than any of us had suspected. Wind of IM’s venture into arthroscopy wafted into the Orthopedics Division long before I set foot for Chicago. One of their members, my chronological peer Ed Wojtys, took it as his crusade to keep me out. He gathered testimony from across the country on what a hazard it would be to let a flea do ‘scopy. Kelley and allies merely asked for a judgement on the adequacy of my training and the competence of my performance. By the end of the year, a plan was in place. I was to perform arthroscopies in the OR while the chief of Orthopedics or a designee watched me and reported back. This would go on for 6 months before judgment would be rendered. In the 6 months prior, I found a friend and savior in Bruce Stubbs. Bruce practiced at the private hospital in town, St. Joe’s, but did his arthroscopies at an affiliate in Chelsea, 15 miles west of Ann Arbor. As a medical student, Bruce had worked in Giles Bole’s lab. Giles was my chief and the guy who took me on as a fellow when no one else would have me. He inspired incredible loyalty in whomever he touched, so when Giles reached out to Bruce to possibly help me out, he readily agreed. I went out to Chelsea once a week and ‘scoped with Bruce. His cases weren’t all arthritis cases, like Bill’s, but practice is practice. Bruce took enormous crap from his peers for this, but was already pretty numb to their criticisms. As one of the first orthopedists in the area to pick up the ‘scope, when its value was pretty much disdained by mainstream orthopedics, he’d learned to go his own way.
I did my first case in U of M’s O.R. 3 days short of Valentine’s day in ’87, a middle aged woman with OA that seemed like it could be something more. During my 6 months in the O.R., I did more arthroscopy cases (5) than the orthopods did (1), rattling off a case a month that first year. I got to fit in, learning the scrub ritual and respecting sterile technique, getting along with the nurses (tho’ Wojtys was said to have “agents”), and enjoying the protection of the anesthesiologist who ran the O.R. schedule, church friend Dave Learned. Once you get those scrubs on, its hard to tell the fleas from the blades
Figure 1. The author arthroscoping a patient in room 16 of U of M’s adult O.R.s
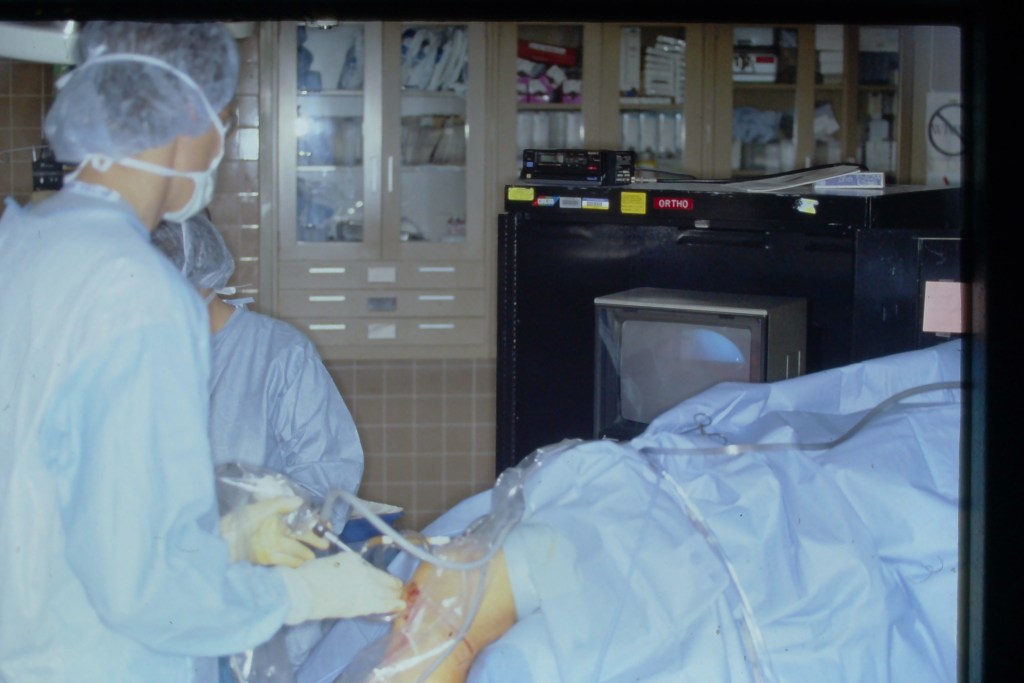
I’d spend a little more than 14 years in the O.R. By ’92, developments in arthroscopy design produced instruments that could be used in a procedure room or clinic setting.
Figure 2. Medical Dynamics fiberoptic needle scope (14 g) inserted into knee at medical procedures unit (not O.R.). Fiberoptics carried light to joint and image back to camera in control box.
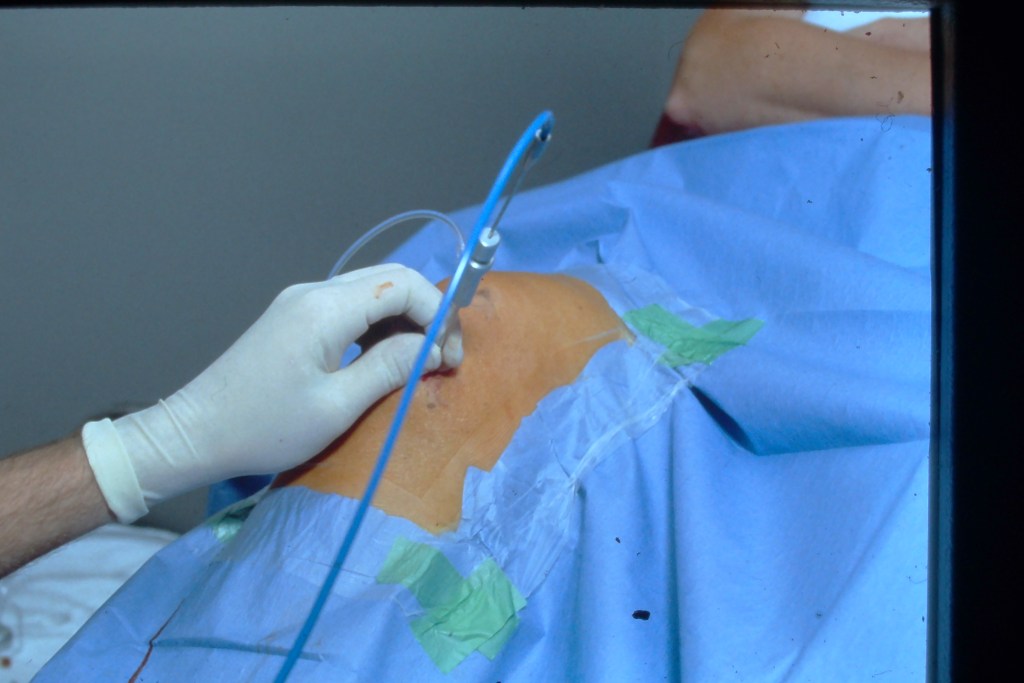
. ‘Scopes for inspection, biopsy, and washout no longer required an O.R., so they saw less and less of this flea. The American College of Rheumatology embraced arthroscopy in the early 90s, sponsoring hands on courses for 3 years which I was one of the faculty, holding an arthroscopy study session at each annual meeting, and supporting research in arthroscopy. But interest waned and the “needle ‘scope” was fragile and after 5 years it no longer produced an acceptable image. The powers that be decided not to repair or upgrade, so it was back to the O.R. Most of the 34 cases I did from then till the end involved major resections: synovectomies or debridements. Meanwhile, evidence was assembled that no arthroscopic interventions into osteoarthritis did more than a placebo (2,3) and the biologic drugs emerging to treat rheumatoid arthritis and other inflammatory arthropathies seemed not to let situations emerge where synovectomy might be considered. So on May 25, 2001, I did my last case and shut out the lights on arthroscopy. I managed to hold my unique spot in the division as the procedures guy, picking up ultrasound, doing all the difficult arthrocenteses and running injection clinics, while doing several bedside biopsies, always teaching others (salivary gland, muscle, skin, synovium).
Then in 2016, I caught wind from an old friend in private practice in Maryland, Nathan Wei (4), about his use of a new 14g needle scope in his office, the MyEye. I visited him and got quite excited about this as a way to resurrect rheumatologic arthroscopy. I was overdue for a sabbatical, so I arranged one with my friend Ken Kalunian at UCSD. He was the guy Bill Arnold trained after me, and had a productive academic career with the ‘scope, tho’ he’d put it down in ’09 and focuses on lupus these days. We’d spend those 3 winter months ‘scoping everyone about to undergo a cortisone injection. Long story short, except for looking at a cadaver knee in a meeting room of a local Marriott, we never touched a ‘scope. His IRB never approved our study, and their credentialling committee never granted me more than observer status. Home, we both tried to get something going, but at each place met fierce opposition from the orthopods, even though we’d never be setting foot in their O.R.s.
That defeat made the go gentle of a semi-forced retirement easier to take. I’m sure if I’d gotten ‘scoping again, I wouldn’t have wanted to put it down. Retirement has given me the opportunity to survey the use of arthroscopy by rheumatologists worldwide. It’s a going thing as a research tool at several institutions, with promise of expansion as examination of synovium becomes ever more important (5). Rheumatologists still have reason to pick up the arthroscope (6), but they should never have to set foot in an O.R. again, making friendship with orthopedists much more likely (7).
References
1. Kelley WN. A new role for the ARA in guiding our destiny. Arthritis Rheum 1987;30(11):1201-4. https://doi: 10.1002/art.1780301101.
2. Moseley JB, O’Malley K, Petersen NJ, Menke TJ, Brody BA, Kuykendall DH, Hollingsworth JC, Ashton CM, Wray NP. A controlled trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med. 2002 Jul 11;347(2):81-8. https://doi: 10.1056/NEJMoa013259.
3. Brignardello-Petersen R, Guyatt GH, Buchbinder R, et al. Knee arthroscopy versus conservative management in patients with degenerative knee disease: a systematic review. BMJ Open 2017;7:e016114. https://doi:10.1136/bmjopen-2017- 016114.
4. Malone DG, Arnold WJ. In memorium: Nathan Wei. The Rheumatologist May 18, 2018. https://www.the-rheumatologist.org/article/in-memoriam-nathan-wei/
5. Ike RW, Arnold WJ, Kalunian KC. Arthroscopy in rheumatology. Where have we been? Where might we go? Rheumatol (Oxford) 2021;60:518–528. Epub 2020 Dec 1 https://doi: 10.1093/rheumatology/keaa560.
6. Ike RW, Kalunian KC. Will rheumatologists ever pick up an arthroscope again? Int J Rheum Dis 2021;24:1235–1246. https://doi: 10.1111/1756-185X.14184
7. Ike RW, Kalunian KC. Regarding arthroscopy: can orthopedists and rheumatologists be friends? J Clin Rheumatol 2021;28:177–181. https://doi: 10.1097/RHU.0000000000001802

Specialist insertion alert. Cardiologists are doing endovascular surgery and causing complications. IR has been doing it a while longer and seem to be causing fewer complications. Per my vascular surgeon buddy.
Anything new has kinks to be worked out.
LikeLike
‘Scopy by rheumas ain’t new. A handful were at it pre-WWII, like Ernst Vauble, who wrote the first book on it. 60s saw rheumas doing ‘scopy in many countries. I first put my toe in the water mid-80s. So nothing really new here, although applications are constantly evolving. However, irrational fear of losing turf and zealous guarding of same is timeless.
LikeLike